|
A gunshot wound (GSW), also known as ballistic trauma, is a form of physical trauma sustained from the discharge of arms or munitions.[3] The most common forms of ballistic trauma stem from firearms used in armed conflicts, civilian sporting, recreational pursuits and criminal activity.[4] Damage is dependent on the firearm, bullet, velocity, entry point, and trajectory. Management can range from observation and local wound care to urgent surgical intervention.
Signs and symptoms[edit]
Trauma from a gunshot wound varies widely based on the bullet, velocity, entry point, trajectory, and affected anatomy. Gunshot wounds can be particularly devastating compared to other penetrating injuries because the trajectory and fragmentation of bullets can be unpredictable after entry. Additionally, gunshot wounds typically involve a large degree of nearby tissue disruption and destruction due to the physical effects of the projectile correlated with the bullet velocity classification.[5]
The immediate damaging effect of a gunshot wound is typically severe bleeding, and with it the potential for hypovolemic shock, a condition characterized by inadequate delivery of oxygen to vital organs. In the case of traumatic hypovolemic shock, this failure of adequate oxygen delivery is due to blood loss, as blood is the means of delivering oxygen to the body's constituent parts. Devastating effects can result when a bullet strikes a vital organ such as the heart, lungs or liver, or damages a component of the central nervous system such as the spinal cord or brain.
Common causes of death following gunshot injury include arterial bleeding, hypoxia caused by pneumothorax, catastrophic injury to the heart and major blood vessels, and damage to the brain or central nervous system. Non-fatal gunshot wounds frequently have mild to severe long-lasting effects, typically some form of major disfigurement such as amputation due to a severe bone fracture, and may cause permanent disability.
Classification[edit]
Gunshot wounds are classified according to the speed of the projectile:
Bullets from handguns are sometimes less than 1,000 ft/s (300 m/s) but with modern pistol loads, they usually are slightly above 1,000 ft/s (300 m/s), while bullets from most modern rifles exceed 2,500 ft/s (760 m/s). One recently developed class of firearm projectiles is the hyper-velocity bullet, such cartridges are usually either wildcats made for achieving such high speed or purpose built factory ammunition with the same goal in mind. Examples of hyper velocity cartridges include the .220 Swift, .17 Remington and .17 Mach IV cartridges. The US military commonly uses 5.56mm bullets, which have a relatively low mass as compared with other bullets (40-62 grains); however, the speed of these bullets is relatively fast (Approximately 2,800 ft/s (850 m/s), placing them in the high velocity category). As a result, they produce a larger amount of kinetic energy, which is transmitted to the tissues of the target.[6] However, one must remember that high kinetic energy does not necessarily equate to high stopping power, as incapacitation usually results from remote wounding effects such as bleeding, rather than raw energy transfer. High energy does indeed result in more tissue disruption, which plays a role in incapacitation, but other factors such as wound size and shot placement play as big of, if not a bigger role in stopping power and thus, effectiveness. Muzzle velocity does not consider the effect of aerodynamic drag on the flight of the bullet for the sake of ease of comparison.
Physics[edit]
The degree of tissue disruption caused by a projectile is related to the cavitation the projectile creates as it passes through tissue. A bullet with sufficient energy will have a cavitation effect in addition to the penetrating track injury. As the bullet passes through the tissue, initially crushing then lacerating, the space left forms a cavity; this is called the permanent cavity. Higher-velocity bullets create a pressure wave that forces the tissues away, creating not only a permanent cavity the size of the caliber of the bullet but also a temporary cavity or secondary cavity, which is often many times larger than the bullet itself.[6] The temporary cavity is the radial stretching of tissue around the bullet's wound track, which momentarily leaves an empty space caused by high pressures surrounding the projectile that accelerate material away from its path.[7] The extent of cavitation, in turn, is related to the following characteristics of the projectile:
Management[edit]Workup[edit]
Initial workup for a gunshot wound is approached in the same way as any acute trauma case. A rapid first pass of the person is conducted using advanced trauma life support (ATLS) protocol in order to ensure that the most vital functions are intact.[9] These include:
Depending on the extent of injury, management can range from urgent surgical intervention to observation. As such, any history from the scene such as gun type, shots fired, shot direction and distance, blood loss on scene, and pre-hospital vitals signs can be very helpful in directing management. Unstable people with signs of bleeding that cannot be controlled during the initial evaluation require immediate surgical exploration in the operating room.[9] Otherwise, management protocols are generally dictated by anatomic entry point and anticipated trajectory.
Neck[edit]
A gunshot wound to the neck can be particularly dangerous because of the high number of vital anatomical structures contained within a small space. The neck contains the larynx, trachea, pharynx, esophagus, vasculature (carotid, subclavian, and vertebral arteries; jugular, brachiocephalic, and vertebral veins; thyroid vessels), and nervous system anatomy (spinal cord, cranial nerves, peripheral nerves, sympathetic chain, brachial plexus). Gunshots to the neck can thus cause severe bleeding, airway compromise, and nervous system injury.[10]
Initial assessment of a gunshot wound to the neck involves non-probing inspection of whether the injury is a penetrating neck injury (PNI), classified by violation of the platsyma muscle.[10] If the platsyma is intact, the wound is considered superficial and only requires local wound care. If the injury is a PNI, surgery should be consulted immediately while the case is being managed. Of note, wounds should not be explored on the field or in the emergency department given the risk of exacerbating the wound.
Penetrating Neck Injury Protocol. Adapted from PMID23317595.
Due to the advances in diagnostic imaging, management of PNI has been shifting from a 'zone-based' approach, which uses anatomical site of injury to guide decisions, to a 'no-zone' approach which uses a symptom-based algorithm.[11] The no-zone approach uses a hard signs and imaging system to guide next steps. Hard signs include airway compromise, unresponsive shock, diminished pulses, uncontrolled bleeding, expanding hematoma, bruits/thrill, air bubbling from wound or extensive subcutaneous air, stridor/hoarseness, neurological deficits.[11] If any hard signs are present, immediate surgical exploration and repair is pursued alongside airway and bleeding control. If there are no hard signs, the person receives a multi-detector CT angiography for better diagnosis. A directed angiography or endoscopy may be warranted in a high-risk trajectory for the gunshot. A positive finding on CT leads to operative exploration. If negative, the person may be observed with local wound care.[11]
Chest[edit]
Important anatomy in the chest includes the chest wall, ribs, spine, spinal cord, intercostal neurovascular bundles, lungs, bronchi, heart, aorta, major vessels, esophagus, thoracic duct, and diaphragm. Gunshots to the chest can thus cause severe bleeding (hemothorax), respiratory compromise (pneumothorax, hemothorax, pulmonary contusion, tracheobronchial injury), cardiac injury (pericardial tamponade), esophageal injury, and nervous system injury.[12]
Initial workup as outlined in the Workup section is particularly important with gunshot wounds to the chest because of the high risk for direct injury to the lungs, heart, and major vessels. Important notes for the initial workup specific for chest injuries are as follows. In people with pericardial tamponade or tension pneumothorax, the chest should be evacuated or decompressed if possible prior to attempting tracheal intubation because the positive pressure ventilation can cause hypotention or cardiovascular collapse.[13] Those with signs of a tension pneumothorax (asymmetric breathing, unstable blood flow, respiratory distress) should immediately receive a chest tube (> French 36) or needle decompression if chest tube placement is delayed.[13] FAST exam should include extended views into the chest to evaluate for hemopericardium, pneumothorax, hemothorax, and peritoneal fluid.[13]
Those with cardiac tamponade, uncontrolled bleeding, or a persistent air leak from a chest tube all require surgery.[14] Cardiac tamponade can be identified on FAST exam. Blood loss warranting surgery is 1-1.5 L of immediate chest tube drainage or ongoing bleeding of 200-300 mL/hr.[14][15] Persistent air leak is suggestive of tracheobronchial injury which will not heal without surgical intervention.[14] Depending on the severity of the person's condition and if cardiac arrest is recent or imminent, the person may require surgical intervention in the emergency department, otherwise known as an emergency department thoracotomy (EDT).[16]
However, not all gunshot to the chest require surgery. Asymptomatic people with a normal chest X-ray can be observed with a repeat exam and imaging after 6 hours to ensure no delayed development of pneumothorax or hemothorax.[13] If a person only has a pneumothorax or hemothorax, a chest tube is usually sufficient for management unless there is large volume bleeding or persistent air leak as noted above.[13] Additional imaging after initial chest X-ray and ultrasound can be useful in guiding next steps for stable people. Common imaging modalities include chest CT, formal echocardiography, angiography, esophagoscopy, esophagography, and bronchoscopy depending on the signs and symptoms.[17]
Abdomen[edit]
Abdominal gunshot wound
Important anatomy in the abdomen includes the stomach, small bowel, colon, liver, spleen, pancreas, kidneys, spine, diaphragm, descending aorta, and other abdominal vessels and nerves. Gunshots to the abdomen can thus cause severe bleeding, release of bowel contents, peritonitis, organ rupture, respiratory compromise, and neurological deficits.
The most important initial evaluation of a gunshot wound to the abdomen is whether there is uncontrolled bleeding, inflammation of the peritoneum, or spillage of bowel contents. If any of these are present, the person should be transferred immediately to the operating room for laparotomy.[18] If it is difficult to evaluate for those indications because the person is unresponsive or incomprehensible, it is up to the surgeon's discretion whether to pursue laparotomy, exploratory laparoscopy, or alternative investigative tools.
Although all people with abdominal gunshot wounds were taken to the operating room in the past, practice has shifted in recent years with the advances in imaging to non-operative approaches in more stable people.[19] If the person's vital signs are stable without indication for immediate surgery, imaging is done to determine the extent of injury.[19]Ultrasound (FAST) and help identify intra-abdominal bleeding and X-rays can help determine bullet trajectory and fragmentation.[19] However, the best and preferred mode of imaging is high-resolution multi-detector CT (MDCT) with IV, oral, and sometimes rectal contrast.[19] Severity of injury found on imaging will determine whether the surgeon takes an operative or close observational approach.
Diagnostic peritoneal lavage (DPL) has become largely obsolete with the advances in MDCT, with use limited to centers without access to CT to guide requirement for urgent transfer for operation.[19]
Extremities[edit]
Acute penetrating trauma from a close-range shotgun blast injury to knee. Birdshot pellets are visible in the wound, within the shattered patella. The powder wad from the shotgun shell has been extracted from the wound, and is visible at the upper right of the image.
The four main components of extremities are bones, vessels, nerves, and soft tissues. Gunshot wounds can thus cause severe bleeding, fractures, nerve deficits, and soft tissue damage. The Mangled Extremity Severity Score (MESS) is used to classify the severity of injury and evaluates for severity of skeletal and/or soft tissue injury, limb ischemia, shock, and age.[20] Depending on the extent of injury, management can range from superficial wound care to limb amputation.
Vital sign stability and vascular assessment are the most important determinants of management in extremity injuries. As with other traumatic cases, those with uncontrolled bleeding require immediate surgical intervention.[9] If surgical intervention is not readily available and direct pressure is insufficient to control bleeding, tourniquets or direct clamping of visible vessels may be used temporarily to slow active bleeding.[21] People with hard signs of vascular injury also require immediate surgical intervention. Hard signs include active bleeding, expanding or pulsatile hematoma, bruit/thrill, absent distal pulses and signs of extremity ischemia.[22]
For stable people without hard signs of vascular injury, an injured extremity index (IEI) should be calculated by comparing the blood pressure in the injured limb compared to an uninjured limb in order to further evaluate for potential vascular injury.[23] If the IEI or clinical signs are suggestive of vascular injury, the person may undergo surgery or receive further imaging including CT angiography or conventional arteriography.
In addition to vascular management, people must be evaluated for bone, soft tissue, and nerve injury. Plain films can be used for fractures alongside CTs for soft tissue assessment. Fractures must be debrided and stabilized, nerves repaired when possible, and soft tissue debrided and covered.[24] This process can often require multiple procedures over time depending on the severity of injury.
Epidemiology[edit]Gunshot Entry And Exit Wounds Test
Assault by firearm resulted in 173,000 deaths globally in 2015, up from 128,000 deaths in 1990.[2][25] Additionally, there were 32,000 unintentional firearm deaths in 2015.[2] As of 2016, the countries with the highest rates of gun violence per capita were El Salvador, Venezuela, and Guatemala with 40.3, 34.8, and 26.8 violent gun deaths per 100,000 people respectively.[26] The countries with the lowest rates of were Singapore, Japan, and South Korea with 0.03, 0.04, and 0.05 violent gun deaths per 100,000 people respectively.[26]
United States[edit]
The United States has the 31st highest rate of violent gun deaths in the world with 3.85 deaths per 100,000 people in 2016.[26] The majority of all homicides and suicides are firearm-related, and the majority of firearm-related deaths are the result of murder and suicide.[27] When sorted by GDP, however, the United States has a much higher violent gun death rate compared to other developed countries, with over 10 times the number of firearms assault deaths than the next four highest GDP countries combined.[28] Gunshot violence is the third most costly cause of injury and the fourth most expensive form of hospitalization in the United States.[29]
History[edit]
Hieronymus Brunschwig argued that infection of gunshot wounds was a result of poisoning by gunpowder, which provided the rationale for cauterizing wounds. Ambroise Paré wrote in his 1545 book, The Method of Curing Wounds Caused by Arquebus and Firearms, that wounds should be sealed rather than cauterized.[30][31]John Hunter argued that infection was not caused by poisoning.
Until the 1880s, the standard practice for treating a gunshot wound called for physicians to insert their unsterilized fingers into the wound to probe and locate the path of the bullet.[32] Surgically opening abdominal cavities to repair gunshot wounds,[33]germ theory, and Joseph Lister's technique for antiseptic surgery using diluted carbolic acid, first demonstrated in 1865, had not yet been accepted as standard practice. For example, sixteen doctors attended to President James A. Garfield after he was shot, and most probed the wound with their fingers or dirty instruments.[34] Historians agree that massive infection was a significant factor in Garfield's death.[32][35]
At almost the same time, in Tombstone, Arizona Territory, on 13 July 1881, George E. Goodfellow performed the first laparotomy to treat an abdominal gunshot wound.[36]:M-9 Goodfellow pioneered the use of sterile techniques in treating gunshot wounds,[37] washing the person's wound and his hands with lye soap or whisky.[38] He became America's leading authority on gunshot wounds[39] and is credited as the United States' first civilian trauma surgeon.[40]
Today's surgeons consider any projectile with a velocity of 330 m/s to be low or subsonic and practically all modern weapons have bullet speeds that are usually higher (for example, a 124 grain 9mm bullet fired from a 4-inch barrel has a velocity of roughly 350 m/s). By contrast, mid-nineteenth-century handguns such as the Colt revolvers used during the American Civil War had muzzle velocities of just 230–260 m/s and their powder and ball predecessors had velocities of 167 m/s or less. Many of these weapons were still in circulation in America during the 1860s. Unlike today's high-velocity bullets, nineteenth-century balls produced almost little or no cavitation (a kinetic shockwave that causes serious tissue damage) and, being slower moving, they were liable to lodge in unusual locations at odds with their trajectory.[41]
Wilhelm Röntgen's discovery of X-rays in 1895 led to the use of radiographs to locate bullets in wounded soldiers.[30]
Survival rates for gunshot wounds improved among US military personnel during the Korean and Vietnam Wars, due in part to helicopter evacuation, along with improvements in resuscitation and battlefield medicine.[30][42] Similar improvements were seen in US trauma practices during the Iraq War.[43] Some military trauma care practices are disseminated by citizen soldiers who return to civilian practice.[30][44][45] One such practice is to transfer major trauma cases to an operating theater as soon as possible, to stop internal bleeding. Within the United States, the survival rate for gunshot wounds has increased, leading to apparent declines in the gun death rate in states that have stable rates of gunshot hospitalizations.[46][47][48][49]
Research[edit]
Research into gunshot wounds is hampered by lack of funding. Federal-funded research into firearm injury, epidemiology, violence, and prevention is minimal. Pressure from the National Rifle Association, the gun lobby, and some gun owners, expressing concerns regarding increased government controls on freedom and guns, is highly effective in preventing related research.[6]
References[edit]
Bibliography[edit]
External links[edit]
Retrieved from 'https://en.wikipedia.org/w/index.php?title=Gunshot_wound&oldid=904212178'
(Redirected from Ballistic trauma)
Signs and symptoms[edit]
Trauma from a gunshot wound varies widely based on the bullet, velocity, entry point, trajectory, and affected anatomy. Gunshot wounds can be particularly devastating compared to other penetrating injuries because the trajectory and fragmentation of bullets can be unpredictable after entry. Additionally, gunshot wounds typically involve a large degree of nearby tissue disruption and destruction due to the physical effects of the projectile correlated with the bullet velocity classification.[5]
The immediate damaging effect of a gunshot wound is typically severe bleeding, and with it the potential for hypovolemic shock, a condition characterized by inadequate delivery of oxygen to vital organs. In the case of traumatic hypovolemic shock, this failure of adequate oxygen delivery is due to blood loss, as blood is the means of delivering oxygen to the body's constituent parts. Devastating effects can result when a bullet strikes a vital organ such as the heart, lungs or liver, or damages a component of the central nervous system such as the spinal cord or brain.
Common causes of death following gunshot injury include arterial bleeding, hypoxia caused by pneumothorax, catastrophic injury to the heart and major blood vessels, and damage to the brain or central nervous system. Non-fatal gunshot wounds frequently have mild to severe long-lasting effects, typically some form of major disfigurement such as amputation due to a severe bone fracture, and may cause permanent disability.
Classification[edit]
Gunshot wounds are classified according to the speed of the projectile:
Bullets from handguns are sometimes less than 1,000 ft/s (300 m/s) but with modern pistol loads, they usually are slightly above 1,000 ft/s (300 m/s), while bullets from most modern rifles exceed 2,500 ft/s (760 m/s). One recently developed class of firearm projectiles is the hyper-velocity bullet, such cartridges are usually either wildcats made for achieving such high speed or purpose built factory ammunition with the same goal in mind. Examples of hyper velocity cartridges include the .220 Swift, .17 Remington and .17 Mach IV cartridges. The US military commonly uses 5.56mm bullets, which have a relatively low mass as compared with other bullets (40-62 grains); however, the speed of these bullets is relatively fast (Approximately 2,800 ft/s (850 m/s), placing them in the high velocity category). As a result, they produce a larger amount of kinetic energy, which is transmitted to the tissues of the target.[6] However, one must remember that high kinetic energy does not necessarily equate to high stopping power, as incapacitation usually results from remote wounding effects such as bleeding, rather than raw energy transfer. High energy does indeed result in more tissue disruption, which plays a role in incapacitation, but other factors such as wound size and shot placement play as big of, if not a bigger role in stopping power and thus, effectiveness. Muzzle velocity does not consider the effect of aerodynamic drag on the flight of the bullet for the sake of ease of comparison.
Physics[edit]
The degree of tissue disruption caused by a projectile is related to the cavitation the projectile creates as it passes through tissue. A bullet with sufficient energy will have a cavitation effect in addition to the penetrating track injury. As the bullet passes through the tissue, initially crushing then lacerating, the space left forms a cavity; this is called the permanent cavity. Higher-velocity bullets create a pressure wave that forces the tissues away, creating not only a permanent cavity the size of the caliber of the bullet but also a temporary cavity or secondary cavity, which is often many times larger than the bullet itself.[6] The temporary cavity is the radial stretching of tissue around the bullet's wound track, which momentarily leaves an empty space caused by high pressures surrounding the projectile that accelerate material away from its path.[7] The extent of cavitation, in turn, is related to the following characteristics of the projectile:
Management[edit]Workup[edit]
Initial workup for a gunshot wound is approached in the same way as any acute trauma case. A rapid first pass of the person is conducted using advanced trauma life support (ATLS) protocol in order to ensure that the most vital functions are intact.[9] These include:
Depending on the extent of injury, management can range from urgent surgical intervention to observation. As such, any history from the scene such as gun type, shots fired, shot direction and distance, blood loss on scene, and pre-hospital vitals signs can be very helpful in directing management. Unstable people with signs of bleeding that cannot be controlled during the initial evaluation require immediate surgical exploration in the operating room.[9] Otherwise, management protocols are generally dictated by anatomic entry point and anticipated trajectory.
Neck[edit]
A gunshot wound to the neck can be particularly dangerous because of the high number of vital anatomical structures contained within a small space. The neck contains the larynx, trachea, pharynx, esophagus, vasculature (carotid, subclavian, and vertebral arteries; jugular, brachiocephalic, and vertebral veins; thyroid vessels), and nervous system anatomy (spinal cord, cranial nerves, peripheral nerves, sympathetic chain, brachial plexus). Gunshots to the neck can thus cause severe bleeding, airway compromise, and nervous system injury.[10]
Initial assessment of a gunshot wound to the neck involves non-probing inspection of whether the injury is a penetrating neck injury (PNI), classified by violation of the platsyma muscle.[10] If the platsyma is intact, the wound is considered superficial and only requires local wound care. If the injury is a PNI, surgery should be consulted immediately while the case is being managed. Of note, wounds should not be explored on the field or in the emergency department given the risk of exacerbating the wound.
Penetrating Neck Injury Protocol. Adapted from PMID23317595.
Due to the advances in diagnostic imaging, management of PNI has been shifting from a 'zone-based' approach, which uses anatomical site of injury to guide decisions, to a 'no-zone' approach which uses a symptom-based algorithm.[11] The no-zone approach uses a hard signs and imaging system to guide next steps. Hard signs include airway compromise, unresponsive shock, diminished pulses, uncontrolled bleeding, expanding hematoma, bruits/thrill, air bubbling from wound or extensive subcutaneous air, stridor/hoarseness, neurological deficits.[11] If any hard signs are present, immediate surgical exploration and repair is pursued alongside airway and bleeding control. If there are no hard signs, the person receives a multi-detector CT angiography for better diagnosis. A directed angiography or endoscopy may be warranted in a high-risk trajectory for the gunshot. A positive finding on CT leads to operative exploration. If negative, the person may be observed with local wound care.[11]
Chest[edit]
Important anatomy in the chest includes the chest wall, ribs, spine, spinal cord, intercostal neurovascular bundles, lungs, bronchi, heart, aorta, major vessels, esophagus, thoracic duct, and diaphragm. Gunshots to the chest can thus cause severe bleeding (hemothorax), respiratory compromise (pneumothorax, hemothorax, pulmonary contusion, tracheobronchial injury), cardiac injury (pericardial tamponade), esophageal injury, and nervous system injury.[12]
Initial workup as outlined in the Workup section is particularly important with gunshot wounds to the chest because of the high risk for direct injury to the lungs, heart, and major vessels. Important notes for the initial workup specific for chest injuries are as follows. In people with pericardial tamponade or tension pneumothorax, the chest should be evacuated or decompressed if possible prior to attempting tracheal intubation because the positive pressure ventilation can cause hypotention or cardiovascular collapse.[13] Those with signs of a tension pneumothorax (asymmetric breathing, unstable blood flow, respiratory distress) should immediately receive a chest tube (> French 36) or needle decompression if chest tube placement is delayed.[13] FAST exam should include extended views into the chest to evaluate for hemopericardium, pneumothorax, hemothorax, and peritoneal fluid.[13]
Those with cardiac tamponade, uncontrolled bleeding, or a persistent air leak from a chest tube all require surgery.[14] Cardiac tamponade can be identified on FAST exam. Blood loss warranting surgery is 1-1.5 L of immediate chest tube drainage or ongoing bleeding of 200-300 mL/hr.[14][15] Persistent air leak is suggestive of tracheobronchial injury which will not heal without surgical intervention.[14] Depending on the severity of the person's condition and if cardiac arrest is recent or imminent, the person may require surgical intervention in the emergency department, otherwise known as an emergency department thoracotomy (EDT).[16]
However, not all gunshot to the chest require surgery. Asymptomatic people with a normal chest X-ray can be observed with a repeat exam and imaging after 6 hours to ensure no delayed development of pneumothorax or hemothorax.[13] If a person only has a pneumothorax or hemothorax, a chest tube is usually sufficient for management unless there is large volume bleeding or persistent air leak as noted above.[13] Additional imaging after initial chest X-ray and ultrasound can be useful in guiding next steps for stable people. Common imaging modalities include chest CT, formal echocardiography, angiography, esophagoscopy, esophagography, and bronchoscopy depending on the signs and symptoms.[17]
Abdomen[edit]
Abdominal gunshot wound
Important anatomy in the abdomen includes the stomach, small bowel, colon, liver, spleen, pancreas, kidneys, spine, diaphragm, descending aorta, and other abdominal vessels and nerves. Gunshots to the abdomen can thus cause severe bleeding, release of bowel contents, peritonitis, organ rupture, respiratory compromise, and neurological deficits.
The most important initial evaluation of a gunshot wound to the abdomen is whether there is uncontrolled bleeding, inflammation of the peritoneum, or spillage of bowel contents. If any of these are present, the person should be transferred immediately to the operating room for laparotomy.[18] If it is difficult to evaluate for those indications because the person is unresponsive or incomprehensible, it is up to the surgeon's discretion whether to pursue laparotomy, exploratory laparoscopy, or alternative investigative tools.
Although all people with abdominal gunshot wounds were taken to the operating room in the past, practice has shifted in recent years with the advances in imaging to non-operative approaches in more stable people.[19] If the person's vital signs are stable without indication for immediate surgery, imaging is done to determine the extent of injury.[19]Ultrasound (FAST) and help identify intra-abdominal bleeding and X-rays can help determine bullet trajectory and fragmentation.[19] However, the best and preferred mode of imaging is high-resolution multi-detector CT (MDCT) with IV, oral, and sometimes rectal contrast.[19] Severity of injury found on imaging will determine whether the surgeon takes an operative or close observational approach.
Diagnostic peritoneal lavage (DPL) has become largely obsolete with the advances in MDCT, with use limited to centers without access to CT to guide requirement for urgent transfer for operation.[19]
Extremities[edit]
Acute penetrating trauma from a close-range shotgun blast injury to knee. Birdshot pellets are visible in the wound, within the shattered patella. The powder wad from the shotgun shell has been extracted from the wound, and is visible at the upper right of the image.
The four main components of extremities are bones, vessels, nerves, and soft tissues. Gunshot wounds can thus cause severe bleeding, fractures, nerve deficits, and soft tissue damage. The Mangled Extremity Severity Score (MESS) is used to classify the severity of injury and evaluates for severity of skeletal and/or soft tissue injury, limb ischemia, shock, and age.[20] Depending on the extent of injury, management can range from superficial wound care to limb amputation.
Vital sign stability and vascular assessment are the most important determinants of management in extremity injuries. As with other traumatic cases, those with uncontrolled bleeding require immediate surgical intervention.[9] If surgical intervention is not readily available and direct pressure is insufficient to control bleeding, tourniquets or direct clamping of visible vessels may be used temporarily to slow active bleeding.[21] People with hard signs of vascular injury also require immediate surgical intervention. Hard signs include active bleeding, expanding or pulsatile hematoma, bruit/thrill, absent distal pulses and signs of extremity ischemia.[22]
For stable people without hard signs of vascular injury, an injured extremity index (IEI) should be calculated by comparing the blood pressure in the injured limb compared to an uninjured limb in order to further evaluate for potential vascular injury.[23] If the IEI or clinical signs are suggestive of vascular injury, the person may undergo surgery or receive further imaging including CT angiography or conventional arteriography.
In addition to vascular management, people must be evaluated for bone, soft tissue, and nerve injury. Plain films can be used for fractures alongside CTs for soft tissue assessment. Fractures must be debrided and stabilized, nerves repaired when possible, and soft tissue debrided and covered.[24] This process can often require multiple procedures over time depending on the severity of injury.
Epidemiology[edit]
Assault by firearm resulted in 173,000 deaths globally in 2015, up from 128,000 deaths in 1990.[2][25] Additionally, there were 32,000 unintentional firearm deaths in 2015.[2] As of 2016, the countries with the highest rates of gun violence per capita were El Salvador, Venezuela, and Guatemala with 40.3, 34.8, and 26.8 violent gun deaths per 100,000 people respectively.[26] The countries with the lowest rates of were Singapore, Japan, and South Korea with 0.03, 0.04, and 0.05 violent gun deaths per 100,000 people respectively.[26]
United States[edit]
The United States has the 31st highest rate of violent gun deaths in the world with 3.85 deaths per 100,000 people in 2016.[26] The majority of all homicides and suicides are firearm-related, and the majority of firearm-related deaths are the result of murder and suicide.[27] When sorted by GDP, however, the United States has a much higher violent gun death rate compared to other developed countries, with over 10 times the number of firearms assault deaths than the next four highest GDP countries combined.[28] Gunshot violence is the third most costly cause of injury and the fourth most expensive form of hospitalization in the United States.[29]
History[edit]
Hieronymus Brunschwig argued that infection of gunshot wounds was a result of poisoning by gunpowder, which provided the rationale for cauterizing wounds. Ambroise Paré wrote in his 1545 book, The Method of Curing Wounds Caused by Arquebus and Firearms, that wounds should be sealed rather than cauterized.[30][31]John Hunter argued that infection was not caused by poisoning.
Until the 1880s, the standard practice for treating a gunshot wound called for physicians to insert their unsterilized fingers into the wound to probe and locate the path of the bullet.[32] Surgically opening abdominal cavities to repair gunshot wounds,[33]germ theory, and Joseph Lister's technique for antiseptic surgery using diluted carbolic acid, first demonstrated in 1865, had not yet been accepted as standard practice. For example, sixteen doctors attended to President James A. Garfield after he was shot, and most probed the wound with their fingers or dirty instruments.[34] Historians agree that massive infection was a significant factor in Garfield's death.[32][35]
At almost the same time, in Tombstone, Arizona Territory, on 13 July 1881, George E. Goodfellow performed the first laparotomy to treat an abdominal gunshot wound.[36]:M-9 Goodfellow pioneered the use of sterile techniques in treating gunshot wounds,[37] washing the person's wound and his hands with lye soap or whisky.[38] He became America's leading authority on gunshot wounds[39] and is credited as the United States' first civilian trauma surgeon.[40]
Today's surgeons consider any projectile with a velocity of 330 m/s to be low or subsonic and practically all modern weapons have bullet speeds that are usually higher (for example, a 124 grain 9mm bullet fired from a 4-inch barrel has a velocity of roughly 350 m/s). By contrast, mid-nineteenth-century handguns such as the Colt revolvers used during the American Civil War had muzzle velocities of just 230–260 m/s and their powder and ball predecessors had velocities of 167 m/s or less. Many of these weapons were still in circulation in America during the 1860s. Unlike today's high-velocity bullets, nineteenth-century balls produced almost little or no cavitation (a kinetic shockwave that causes serious tissue damage) and, being slower moving, they were liable to lodge in unusual locations at odds with their trajectory.[41]
Wilhelm Röntgen's discovery of X-rays in 1895 led to the use of radiographs to locate bullets in wounded soldiers.[30]
Survival rates for gunshot wounds improved among US military personnel during the Korean and Vietnam Wars, due in part to helicopter evacuation, along with improvements in resuscitation and battlefield medicine.[30][42] Similar improvements were seen in US trauma practices during the Iraq War.[43] Some military trauma care practices are disseminated by citizen soldiers who return to civilian practice.[30][44][45] One such practice is to transfer major trauma cases to an operating theater as soon as possible, to stop internal bleeding. Within the United States, the survival rate for gunshot wounds has increased, leading to apparent declines in the gun death rate in states that have stable rates of gunshot hospitalizations.[46][47][48][49]
Research[edit]
Research into gunshot wounds is hampered by lack of funding. Federal-funded research into firearm injury, epidemiology, violence, and prevention is minimal. Pressure from the National Rifle Association, the gun lobby, and some gun owners, expressing concerns regarding increased government controls on freedom and guns, is highly effective in preventing related research.[6]
References[edit]
Bibliography[edit]
External links[edit]
Retrieved from 'https://en.wikipedia.org/w/index.php?title=Gunshot_wound&oldid=904212178'
Published online 2015 Nov 4. doi: 10.1186/s13017-015-0048-z
PMID: 26561497
Abstract
The presence at CT scan of more retained bullets than expected could be a very difficult interpretation challenge in the early management of gunshot wounds. The modern non operative management of haemodinamically stable patients without peritonitis requires that the trajectory of the bullet is clearly recognized. This clinical case reporting of a gunshot wound without evident entry hole, allows to discuss the diagnostic and therapeutic implications in the management of gunshot wounds cases with atypical entry and/or exit holes.
Keywords: Gunshot, Atypical inlet hole, Intestinal perforation, Diagnosis, Laparotomy, Laparoscopy
Background
In case of abdominal gunshot wound, exploratory surgery has always been deemed indicated, as the likelihood that the bullet has caused a perforation of the gastrointestinal tract is high; unlike the lesions of solid organs, characterized by haemoperitoneum easily detectable by CT scan, intestinal perforation may not be immediately recognized, especially when the CT is carried out quickly, so that the air contained in the bowel has not the time to go outside and to be recorded as an indirect sign of perforation. However some Authors have recently proposed a more selective indication for surgery, based on serial CTs, in cases where the first CT is negative and the patient is haemodinamically stable, with the aim of avoiding unnecessary laparotomies. Two recently published papers highlight the role of laparoscopy in non-operative management of abdominal gunshot wounds, expecially when clinic is not clear or in presence of peritoneal signs [, ].
Hotline miami a+ scores. Obviously a quite different problem arises when entry and/or exit holes of the bullets are not clearly detectable, as highlighted by the reported singular case of unrecognized gunshot entrance hole, due to the fact that the patient was shot through his anus. To our best knowledge in scientific Literature there is any case of undetected entrance hole due to trans-anal gunshot, even if we found out 2 rare cases of unrecognized gastrointestinal bullet embolism [–]. We think that the reported case could be helpful to better understand the problem of unrecognized abdominal injuries following traumas.
Case presentation
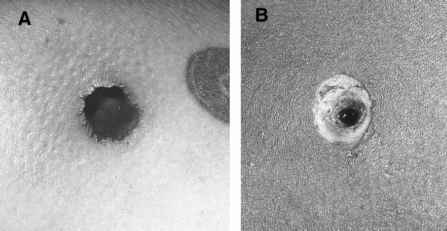
The Patient, a 60-years old Caucasian male found unconscious in a trailer park of gypsies, was carried to Emergency Department at night, intubated and haemodynamically stable. At physical examination he presented a head gunshot wound, with an only visible bullet-hole located at the back of the neck. No other lesions were found. The total body contrast-enhanced CT scan performed at the Emergency Department revealed a large subdural haematoma, a retained bullet in the brain (Fig. 1) and another retained projectile in the left lung (Fig. 2), without any evidence of thoracic wall wounds; there was no air outside the bowel (Fig. 3a) even if little air bubbles could be recognized near to the pubis (Fig. 3b). These findings were difficult to be interpreted, both by the radiologist, the surgeon and the anaesthesiologist, as patient’s examination performed in the shock room after the CT scan confirmed the only presence of a single bullet-hole located at the back of the neck. As the Patient had no clinical and radiological signs of bowel perforation, it was decided for a “wait-and-see†attitude, scheduling a second CT scan for the following day.
Retained bullet in the brain
Retained projectile in the left lung
a Absence of free air outside the bowel. b Little air bubbles near to the pubis
About 14 h later the second CT scan showed the presence of hematoma near the pubis, peritoneal air bubbles outside the bowel (Fig. 4a, ​,b)b) and diffuse peritoneal free fluid (Fig. 5). These findings were suspected for bowel perforation, thus the patient was translated into operative room: by laparotomy, the haemoperitoneum was drained and multiple perforations of small bowel were identified, associated with a single perforation of the upper part of the rectum, a double perforation of the stomach and a small hole in the left diaphragm, throughout which the bullet had reached the left lung. Multiple sutures of the rectum, the bowel, the stomach and the diaphragm and a small bowel resection were performed; the bulled retained in the lung was not reached nor removed. The only possible explanation for the trajectory of the bullet was that it was shot through the anus; evidently, after the blow on the head, the patient had fallen face down and the assailant shot him throughout the anus. This interpretation was later confirmed by aggressor interrogation by the Police.
a Presence of peritoneal air bubbles outside the bowel. b Hematoma near the pubis
Peritoneal free fluid
The following course of the patient was uneventful; he was estubated after 3 days, having a Glasgow coma scale of 11, and he was discharged to rehabilitation 13 days after the incident; 4 months later the head bullet was removed by anterior approach, while the lung bullet was left in place.
Discussion
From the analysis of this clinical report we concluded that the patient received two gunshot: the first was the only one that could be initially detected and it was fired to the back of the neck, while the second was fired directly throughout the anus; it perforated the rectum, and then it crossed the abdomen causing intestinal, gastric and diaphragmatic perforations, arresting into the left lung. It was not possible to make a correct diagnosis at first observation because a second bullet-hole could not be found.
To our best knowledge no similar cases have been reported in Literature. We only find 2 rare cases of unrecognized bullet embolism in the gastrointestinal tract causing colonic perforation [, ]. In both cases the authors claimed for the importance of accurate patient’s examination, both clinical and radiological in order to avoid delayed diagnosis of visceral injuries. In a paper of Apfelbaum et al. [] the authors highlight the importance of correctly recognizing entrance and exit wounds in the Emergency Department and they admit that it could sometimes be difficult to discriminate the correct type of wound by surgeons. However the authors do not consider about the possibility of unrecognized gunshot wounds due to trans-anal or other natural orifices gunshots.
Many problems in the interpretation and reconstruction of the trajectory of the bullets have been reported in the Literature [, ]; a high index of suspicion should drive the diagnostic work-up, based on knowledge of ballistics and wounding potential of firearms; the goal is to anticipate the severity of a wound and detect earlier occult but severe internal lesions [, ]. In many cases, site of entrance and direction of bullet path could help the clinician to determine the potential of severe internal lesion. However, several singular cases have been described. The most frequent situation are atypical gunshot entrance holes, the wandering bullets, the spent bullet aspiration into the trachea-bronchial tree, and the so called “tandem bulletâ€, in which there are 1 only entry point and more than one exit point, meaning tandem projectiles or multiple projectiles entering through the same hole. Kuy et al. report of undetected urinary tract injuries due to a gunshot wound to the buttock and they also review other similar cases of undetected urinary injuries following gunshot [–]. Another atypical gunshot wound is the one reported from Ro et al., where the patient was shot from his left knee and the bullet travelled subcutaneously until the abdominal cavity perforating the left colon []. The authors highlight the importance of CT scan to accurate evaluation of bullet trajectory, however in this case the trauma team is helped by the presence of well evident entrance hole.
To our knowledge, this is the first report of the absence of an evident entry wound; since the CT scan showed the presence of a retained bullet in the left lung, the search for an entrance hole had been conducted with great attention by the surgeon, the anesthesiologist and the radiologist together. One possible explanation that was proposed was that the bullet had been swallowed and inhaled and then it had taken the path of a segmental bronchu. A second possible explanation was that the pulmonary bullet was fired many times later, during another gunshot assault. Retrospectively reassessing the information available after the first CT scan, the presence of air bubbles and small bone fragments in the extraperitoneal pelvis should have lead to a rectal examination. This was a major missing in the management of the here reported clinical case, even if the absence of indirect signs of bowel perforation was on contrast with the suspicion that the projectile had been shot from the anus and it reached the lung crossing the abdomen.
Performing the rectal examination could have anticipated the understaning of the sequence of the events, but probably the patients management would have not been different, due to his clinical stability and in absence of clinical signs of bowel perforation.
So the decision to repeat the CT scan after a few hours in order to monitor the presence of any sign of possible damage in the peritoneal cavity, was correct as allowed the diagnosis of the intestinal injures before the onset of clinical symptoms, avoiding the patient to die for septic shock [, ]. As an alternative, we could perform a diagnostic laparoscopy, as suggested by newer evidences for abdominal gunshot traumas with clinical suspicion of peritonitis or doubtful clinical signs [, ]; however, once again, our non-operative decision was supported by the stability of the patients, the absence of signs of bowel perforation at the first CT scan and the absence of peritoneal signs.
Conclusion
Firearm wounds are increasingly observed in Emergency Department even in areas with classically low incidence of urban warfare, especially in Europe; they often raise new problems in interpretation both for denial by patients of firearm involvement [] and for atypical clinical presentation []. The possibility of gunshot fired throughout natural orifices, such as anus, should be always taken into account in case of retained bullet without clear entry hole and, more important, the members of the trauma team should always keep in mind that a digital rectal exploration is mandatory in cases of abdominal gunshots wounds with unclear dynamics.
Consent
Written informed consent was obtained from the patient for publication of this Case report and any accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of this journal.
Abbreviations
Footnotes
Competing interests
The authors declare that they have no competing interests.
Authors’ contributions
GB conceived of the study and helped to draft the manuscript. SM carried out the acquisition of data and has been involved in drafting the manuscript. FG has given substantial contribution to interpretations of data. DL carried out the acquisition of data. NP helped participated in study coordination and revised the manuscript critically. All authors read and approved the final manuscript.
Contributor Information
Silvia Ministrini, Phone: ++39 030 3995600, Phone: ++39 030 3390920, Email: [email protected].
Gianluca Baiocchi, Email: [email protected].
Frida Pittiani, Email: moc.liamg@xrhcisp.
Daniele Lomiento, Email: moc.liamtoh@otneimol.
Federico Gheza, Email: ti.liamtoh@azehgedef.
Nazario Portolani, Email: [email protected].
References
1. Navsaria PH1, Nicol AJ, Edu S, Gandhi R, Ball CG. Selective nonoperative management in 1106 patients with abdominal gunshot wounds: conclusions on safety, efficacy, and the role of selective CT imaging in a prospective single-center study. Ann Surg. 2015;261(4):760–4. doi: 10.1097/SLA.0000000000000879. [PubMed] [CrossRef] [Google Scholar]
2. Di Saverio S, Bendinelli C, Coniglio C, Biscardi A, Gordini G, Tugnoli G. The brave challenge of NOM for abdominal GSW trauma and the role of laparoscopy as an alternative to CT scan. Ann Surg. 2015 Jun 23. [Epub ahead of print]. [PubMed]
3. Krispin A, Zaitsev K, Hiss J. The elusive slug: bullet intestinal “embolism†Forensic Sci Med Pathol. 2010;6(4):288–92. doi: 10.1007/s12024-010-9163-z. [PubMed] [CrossRef] [Google Scholar]
4. Saptarshi B, Catherine P, Sunil A. An elusive bullet in the gastrointestinal tract: a rare case of bullet embolism in the gastrointestinal tract and a review of relevant literature. Case Rep Crit Care. 2014;2014:689539.[PMC free article] [PubMed] [Google Scholar]
5. Apfelbaum JD, Shockley LW, Wahe JW, Moore EE. Entrance and exit gunshot wounds: incorrect terms for the emergency department? J Emerg Med. 1998;16(5):741–5. doi: 10.1016/S0736-4679(98)00075-4. [PubMed] [CrossRef] [Google Scholar]
6. Maiden N. Ballistics reviews: mechanisms of bullet wound trauma. Forensic Sci Med Pathol. 2009;5(3):204–9. doi: 10.1007/s12024-009-9096-6. [PubMed] [CrossRef] [Google Scholar]
7. Maiden N. Historical overview of wound ballistics research. Forensic Sci Med Pathol. 2009;5(2):85–9. doi: 10.1007/s12024-009-9090-z. [PubMed] [CrossRef] [Google Scholar]
8. White KM. Injuring mechanisms of gunshot wounds. Crit Care Nurs Clin North Am. 1989;1(1):97–103. [PubMed] [Google Scholar]
9. Fallouh HB, Venugopal PS, Newton A. Occult gunshot wounds in the emergency department. Lancet. 2009;373(9664):631–2. doi: 10.1016/S0140-6736(09)60398-6. [PubMed] [CrossRef] [Google Scholar]
10. Kuy SR, Somberg LB, Paul J, Brown N, Saving A, Codner PA. Undetected penetrating bladder injuries presenting as a spontaneously expulsed bullet during voiding: a rare entity and review of the literature. J Emerg Med. 2013;45(3):e59–e62. doi: 10.1016/j.jemermed.2013.03.039. [PubMed] [CrossRef] [Google Scholar]
11. Cohen SP, Varma KR, Goldman SM. Spontaneous expulsion of intravesical bullet. Urology. 1975;3:387–389. doi: 10.1016/0090-4295(75)90163-6. [PubMed] [CrossRef] [Google Scholar]
12. Abdelsayed MA, Bissada NK, Finkbeiner AE, Redman JF. Spontaneous passage of bullet during voiding. South Med J. 1978;71:83–84. doi: 10.1097/00007611-197801000-00027. [PubMed] [CrossRef] [Google Scholar]
13. Kyriakidis A, Karydis G, Papacharalambous A, Yannopoulos P. Spontaneous passage of shell fragments during voiding. Br J Urol. 1984;56:334. doi: 10.1111/j.1464-410X.1984.tb05403.x. [PubMed] [CrossRef] [Google Scholar]
14. Sankari BR, Parra RO. Spontaneous voiding of a bullet after a gunshot wound to the bladder: case report. J Trauma. 1993;35:813–814. doi: 10.1097/00005373-199311000-00030. [PubMed] [CrossRef] [Google Scholar]
15. DiDomenico D, Guinan P, Sharifi R. Spontaneous expulsion of an intravesical bullet. J Am Osteopath Assoc. 1997;97:415–416. [PubMed] [Google Scholar]
16. Kumar Pal D. Spontaneous passage of shotgun pellets during voiding. Br J Urol. 1998;81:498. doi: 10.1046/j.1464-410x.1998.00576.x. [PubMed] [CrossRef] [Google Scholar]
17. Kilic D, Kilinc F, Ezer A, Guvel S. Spontaneous expulsion of a bullet via the urethra. Int J Urol. 2004;11:567–577. doi: 10.1111/j.1442-2042.2004.00826.x. [PubMed] [CrossRef] [Google Scholar]
18. Ro T, Murray R, Galvan D, Nazim MH. Atypical gunshot wound: bullet trajectory analyzed by computed tomography. Int J Surg Case Rep. 2015;14:104–107. doi: 10.1016/j.ijscr.2015.07.023.[PMC free article] [PubMed] [CrossRef] [Google Scholar]
Articles from World Journal of Emergency Surgery : WJES are provided here courtesy of BioMed Central
(Redirected from Exit Wound)
Penetrating trauma is an injury that occurs when an object pierces the skin and enters a tissue of the body, creating an open wound. In blunt, or non-penetrating trauma, there may be an impact, but the skin is not necessarily broken. The penetrating object may remain in the tissues, come back out the way it entered, or pass through the tissues and exit from another area.[1] An injury in which an object enters the body or a structure and passes all the way through is called a perforating injury, while penetrating trauma implies that the object does not pass through.[2] Perforating trauma is associated with an entrance wound and an often larger exit wound.
Penetrating trauma can be caused by a foreign object or by fragments of a broken bone. Usually occurring in violent crime or armed combat,[3] penetrating injuries are commonly caused by gunshots and stabbings.[4]
Penetrating trauma can be serious because it can damage internal organs and presents a risk of shock and infection. The severity of the injury varies widely depending on the body parts involved, the characteristics of the penetrating object, and the amount of energy transmitted to the tissues.[4] Assessment may involve X-rays or CT scans, and treatment may involve surgery, for example to repair damaged structures or to remove foreign objects. Following penetrating trauma, spinal motion restriction is associated with worse outcomes and therefore its should not be done routinely.[5]
Mechanism[edit]
A gunshot wound
As a missile passes through tissue, it decelerates, dissipating and transferring kinetic energy to the tissues; this is what causes the injury.[1] The velocity of the projectile is a more important factor than its mass in determining how much damage is done;[1] kinetic energy increases with the square of the velocity. In addition to injury caused directly by the object that enters the body, penetrating injuries may be associated with secondary injuries, due for example to a blast injury.[2]
The path of a projectile can be estimated by imagining a line from the entrance wound to the exit wound, but the actual trajectory may vary due to ricochet or differences in tissue density.[4] In a cut, the discolouration and the swelling of the skin from a blow happens because of the ruptured blood vessels and escape of blood and fluid and other injury that interrupts the circulation.[6]
Cavitation[edit]Permanent cavitation[edit]
Low-velocity items, such as knives and swords, are usually propelled by a person's hand, and usually do damage only to the area that is directly contacted by the object.[7] The space left by tissue that is destroyed by the penetrating object as it passes through forms a cavity; this is called permanent cavitation.[8]
Temporary cavitation[edit]
High-velocity objects are usually projectiles such as bullets from high-powered rifles, such as assault rifles[7] or sniper rifles. Bullets classed as medium-velocity projectiles include those from handguns, shotguns,[7] and submachine guns. In addition to causing damage to the tissues they contact, medium- and high-velocity projectiles cause a secondary cavitation injury: as the object enters the body, it creates a pressure wave which forces tissue out of the way, creating a cavity can be much larger than the object itself; this is called temporary cavitation.[8] The temporary cavity is the radial stretching of tissue around the bullet’s wound track, which momentarily leaves an empty space caused by high pressures surrounding the projectile that accelerate material away from its path.[9]
The characteristics of the tissue injured also help determine the severity of the injury; for example, the denser the tissue, the greater the amount of energy transmitted to it.[8] Skin, muscles, and intestines absorb energy and so are resistant to the development of temporary cavitation, while organs such as the liver, spleen, kidney, and brain, which have relatively low tensile strength, are likely to split or shatter because of temporary cavitation.[10] Flexible elastic soft tissues, such as muscle, intestine, skin, and blood vessels, are good energy absorbers and are resistant to tissue stretch. If enough energy is transferred, the liver may disintegrate.[9] Temporary cavitation can be especially damaging when it affects delicate tissues such as the brain, as occurs in penetrating head trauma.[citation needed]
Location[edit]Head[edit]
While penetrating head trauma accounts for only a small percentage of all traumatic brain injuries (TBI), it is associated with a high mortality rate, and only a third of people with penetrating head trauma survive long enough to arrive at a hospital.[11] Injuries from firearms are the leading cause of TBI-related deaths.[11] Penetrating head trauma can cause cerebral contusions and lacerations, intracranial hematomas, pseudoaneurysms, and arteriovenous fistulas.[11] The prognosis for penetrating head injuries varies widely.[11]
Penetrating facial trauma can pose a risk to the airway and breathing; airway obstruction can occur later due to swelling or bleeding.[12] Penetrating eye trauma can cause the globe of the eye to rupture or vitreous humor to leak from it, and presents a serious threat to eyesight.[13]
Chest[edit]
X-ray showing a bullet (white spot) in the heart
Most penetrating injuries are chest wounds and have a mortality rate (death rate) of under 10%.[14] Penetrating chest trauma can injure vital organs such as the heart and lungs and can interfere with breathing and circulation. Lung injuries that can be caused by penetrating trauma include pulmonary laceration (a cut or tear) pulmonary contusion (a bruise), hemothorax (an accumulation of blood in the chest cavity outside of the lung), pneumothorax (an accumulation of air in the chest cavity) and hemopneumothorax (accumulation of both blood and air). Sucking chest wounds and tension pneumothorax may result.
Penetrating trauma can also cause injuries to the heart and circulatory system. When the heart is punctured, it may bleed profusely into the chest cavity if the membrane around it (the pericardium) is significantly torn, or it may cause pericardial tamponade if the pericardium is not disrupted.[15] In pericardial tamponade, blood escapes from the heart but is trapped within the pericardium, so pressure builds up between the pericardium and the heart, compressing the latter and interfering with its pumping.[15]Fractures of the ribs commonly produce penetrating chest trauma when sharp bone ends pierce tissues.
Abdomen[edit]
Penetrating abdominal trauma (PAT) typically arises from stabbings, ballistic injuries (shootings), or industrial accidents.[16] PAT can be life-threatening because abdominal organs, especially those in the retroperitoneal space, can bleed profusely, and the space can hold a large volume of blood.[2] If the pancreas is injured, it may be further injured by its own secretions, in a process called autodigestion.[2] Injuries of the liver, common because of the size and location of the organ, present a serious risk for shock because the liver tissue is delicate and has a large blood supply and capacity.[2] The intestines, taking a large part of the lower abdomen, are also at risk of perforation.
People with penetrating abdominal trauma may have signs of hypovolemic shock (insufficient blood in the circulatory system) and peritonitis (an inflammation of the peritoneum, the membrane that lines the abdominal cavity).[2] Penetration may abolish or diminish bowel sounds due to bleeding, infection, and irritation, and injuries to arteries may cause bruits (a distinctive sound similar to heart murmurs) to be audible.[2] Percussion of the abdomen may reveal hyperresonance (indicating air in the abdominal cavity) or dullness (indicating a buildup of blood).[2] The abdomen may be distended or tender, signs which indicate an urgent need for surgery.[2]
The standard management of penetrating abdominal trauma was for many years mandatory laparotomy. A greater understanding of mechanisms of injury, outcomes from surgery, improved imaging and interventional radiology has led to more conservative operative strategies being adopted.[16]
Assessment and treatment[edit]
Assessment can be difficult because much of the damage is often internal and not visible.[4] The patient is thoroughly examined.[2] X-ray and CT scanning may be used to identify the type and location of potentially lethal injuries.[2] Sometimes before an X-ray is performed on a person with penetrating trauma from a projectile, a paper clip is taped over entry and exit wounds to show their location on the film.[2] The patient is given intravenous fluids to replace lost blood.[2] Surgery may be required; impaled objects are secured into place so that they do not move and cause further injury, and they are removed in an operating room.[2] Foreign bodies such as bullets may be removed, but they may also be left in place if the surgery necessary to get them out would cause more damage than would leaving them.[12] Wounds are debrided to remove tissue that cannot survive and other material that presents risk for infection.[2]
Nnegative pressure wound therapy is no more effective in preventing wound infection than standard care when used on open traumatic wounds.[17]
History[edit]
Ambroise Paré
Before the 17th century, medical practitioners poured hot oil into wounds in order to cauterize damaged blood vessels, but the French surgeon Ambroise Paré challenged the use of this method in 1545.[18] Paré was the first to propose controlling bleeding using ligature.[18]
During the American Civil War, chloroform was used during surgery to reduce pain and allow more time for operations.[2] Due in part to the lack of sterile technique in hospitals, infection was the leading cause of death for wounded soldiers.[2]
In World War I, doctors began replacing patients' lost fluid with salt solutions.[2] With World War II came the idea of blood banking, having quantities of donated blood available to replace lost fluids. The use of antibiotics also came into practice in World War II.[2]
See also[edit]References[edit]
External links[edit]
Retrieved from 'https://en.wikipedia.org/w/index.php?title=Penetrating_trauma&oldid=900090784'
Comments are closed.
|
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
||||||||||||||||||||||||||||||||||||||

 RSS Feed
RSS Feed
